
The Cost Of Artificial Intelligence In Healthcare is an increasingly relevant topic for healthcare leaders, technology providers, and policymakers alike. As artificial intelligence (AI) continues to reshape industries, healthcare stands out as one of the most promising sectors for AI adoption. From diagnosing diseases more accurately to streamlining hospital operations, AI offers the potential to improve patient outcomes while reducing operational inefficiencies.
However, while the benefits are clear, the cost implications of implementing AI in healthcare are often complex and vary widely depending on multiple factors. This raises a crucial question for healthcare providers and investors: how much does it really cost to integrate AI into healthcare services, and is it worth the investment?
The market numbers indicate that the momentum is undeniable. According to Precedence Research, the global AI in healthcare market was valued at $15.1 billion in 2022 and is projected to reach $187.95 billion by 2030. Similarly, Grand View Research estimates the market to hit $187.69 billion by 2030, growing at an impressive 38.6% CAGR between 2025 and 2030. This projected growth reflects a significant shift in healthcare strategies, where AI is no longer viewed as a futuristic tool but a present-day necessity.
At the same time, healthcare costs globally continue to rise. A report by Fierce Healthcare reveals that healthcare expenses are projected to increase by 8% in 2025, further stressing healthcare systems already dealing with resource constraints and workforce burnout.
In this comprehensive guide, we’ll break down the Cost Of Artificial Intelligence In Healthcare, covering:
- The main factors influencing costs
- Real-world cost examples from healthcare AI projects
- Use case-based cost analysis
- ROI and value generated from AI investments
- Strategies to manage and optimize AI expenses
By the end of this guide, healthcare stakeholders will have a clearer understanding of what drives the cost of AI, the value it brings, and whether it’s a strategic investment worth pursuing.
For organizations seeking tailored AI strategies, consulting specialized partners like GlobalNodes ensures that the AI journey is both cost-effective and aligned with healthcare objectives.
What Are the Main Factors Affecting the Cost Of Artificial Intelligence In Healthcare?
The Cost Of Artificial Intelligence In Healthcare is influenced by a variety of factors that determine the scale, complexity, and long-term investment required. Understanding these factors helps healthcare providers plan budgets effectively while ensuring they maximize value from AI deployments.
Let’s explore the core elements that impact the cost of implementing AI in healthcare environments.
Factor 1: The Solution’s Complexity
The more complex the AI solution, the higher the costs involved. A simple AI chatbot designed to answer common patient queries is far less expensive than a sophisticated deep learning model that analyzes radiology images for early disease detection. Complexity affects the amount of data needed, the model sophistication, and the computational resources required.
Solutions aimed at real-time diagnostics, clinical decision support, or personalized medicine typically require custom models, extensive training, and validation processes—each contributing to higher expenses.
Factor 2: Infrastructure Requirements
AI solutions often demand robust infrastructure, including high-performance computing systems, cloud services, and secure data storage solutions. The costs for infrastructure can vary significantly depending on whether the AI is deployed on-premises or in the cloud.
Cloud-based AI solutions generally reduce upfront hardware costs but involve ongoing subscription and storage fees. Regardless of the deployment model, ensuring data security and compliance with healthcare regulations adds another layer to the infrastructure costs.
For example, organizations exploring machine learning solutions must factor in both computational resources and data processing capabilities, which influence overall investment.
Factor 3: Integration with Existing Healthcare Systems
AI does not operate in isolation; it must integrate with existing electronic health records (EHR), hospital management systems, and other clinical platforms. The Cost Of Artificial Intelligence In Healthcare rises when significant customization or interoperability work is needed to connect AI tools with legacy systems.
Seamless integration ensures that AI delivers actionable insights within current clinical workflows, minimizing disruption while maximizing utility.
Factor 4: AI Implementation Approach
There are multiple pathways to adopting AI in healthcare:
- Off-the-Shelf Solutions: Pre-built AI applications are generally more affordable but may lack customization for specific clinical needs.
- Custom AI Development: Tailored solutions address unique healthcare challenges but come with higher development and testing costs.
- Proof of Concept (PoC): Running a PoC can validate AI viability before full-scale investment, offering a controlled, lower-cost starting point.
Choosing between these approaches directly impacts the budget, time to market, and long-term maintenance commitments.
Factor 5: Data Collection and Training Data Availability
AI models are only as good as the data they’re trained on. Collecting, cleaning, and labeling healthcare data is resource-intensive and often requires specialized teams, especially when dealing with sensitive patient information.
If sufficient quality data is not readily available, organizations might need to invest in synthetic data generation or collaborate with research institutions—both adding to the overall cost.
Factor 6: Regulatory Compliance Costs
Healthcare is one of the most regulated industries, with strict standards like HIPAA in the U.S. and GDPR in Europe dictating how patient data must be handled. Any AI solution deployed in this space must adhere to these compliance requirements, which often means additional investments in security, privacy frameworks, and auditing processes.
Failing to comply can result in significant fines and reputational damage, making compliance not just a cost but a necessity.
How Much Does Artificial Intelligence Cost in Healthcare? Estimates from Our Portfolio
Estimating the Cost Of Artificial Intelligence In Healthcare can be challenging because the price varies based on the solution’s complexity, required infrastructure, and scope of implementation. However, examining real-world projects provides a practical understanding of what healthcare providers might expect to invest when adopting AI.
Below are three examples from healthcare AI projects that illustrate diverse use cases and their associated costs.
Project 1: AI-Powered Telemedicine Solution Cost Breakdown
Telemedicine has become indispensable in modern healthcare, especially with the growing demand for remote consultations and virtual care. One of our projects involved developing an AI-powered telemedicine platform equipped with:
- Intelligent patient triage based on symptoms
- Automated appointment scheduling
- Video consultation capabilities with AI-based transcription support
- Integration with EHR systems for data continuity
Estimated Cost:
Developing a comprehensive telemedicine solution with embedded AI capabilities typically costs between $300,000 to $600,000, depending on features, integrations, and scalability needs.
Much of the cost goes into:
- Custom AI algorithm development
- UI/UX design tailored for both patients and physicians
- Backend infrastructure for secure data handling
- Compliance with healthcare regulations like HIPAA
The platform helped reduce wait times and improved consultation accuracy, offering a significant return on investment by enhancing patient engagement and operational efficiency.
For healthcare providers interested in similar AI-driven scheduling tools, exploring advancements like those discussed in our blog on AI appointment scheduling in healthcare provides valuable insights.
Project 2: AI-Driven Decision Support System for Personalizing Cancer Treatment
Another significant project involved creating an AI-driven decision support system for oncologists. This tool analyzed patient medical histories, genetic data, and clinical research to recommend personalized cancer treatment plans.
Estimated Cost:
Such highly specialized solutions generally range between $500,000 to over $1 million due to:
- The need for advanced machine learning models
- Access to extensive medical datasets
- Continuous model training and validation to ensure accuracy
- Collaboration with medical experts for clinical validation
While the upfront investment is substantial, the system empowered oncologists to deliver precision medicine, enhancing treatment outcomes and reducing trial-and-error approaches in cancer therapy.
Project 3: ML-Driven Web Platform for Calculating Eye Lens Power
In a more targeted application, we developed a machine learning-based web platform designed to assist ophthalmologists in accurately calculating eye lens power for cataract surgery patients.
Features included:
- Input of biometric data for precise calculations
- AI recommendations for lens types
- Integration with clinical records for seamless usage
Estimated Cost:
Developing this focused solution cost around $150,000 to $250,000, reflecting a lower cost compared to broad, multi-functional AI platforms. The limited but high-value scope made this an efficient investment for specialized clinics.
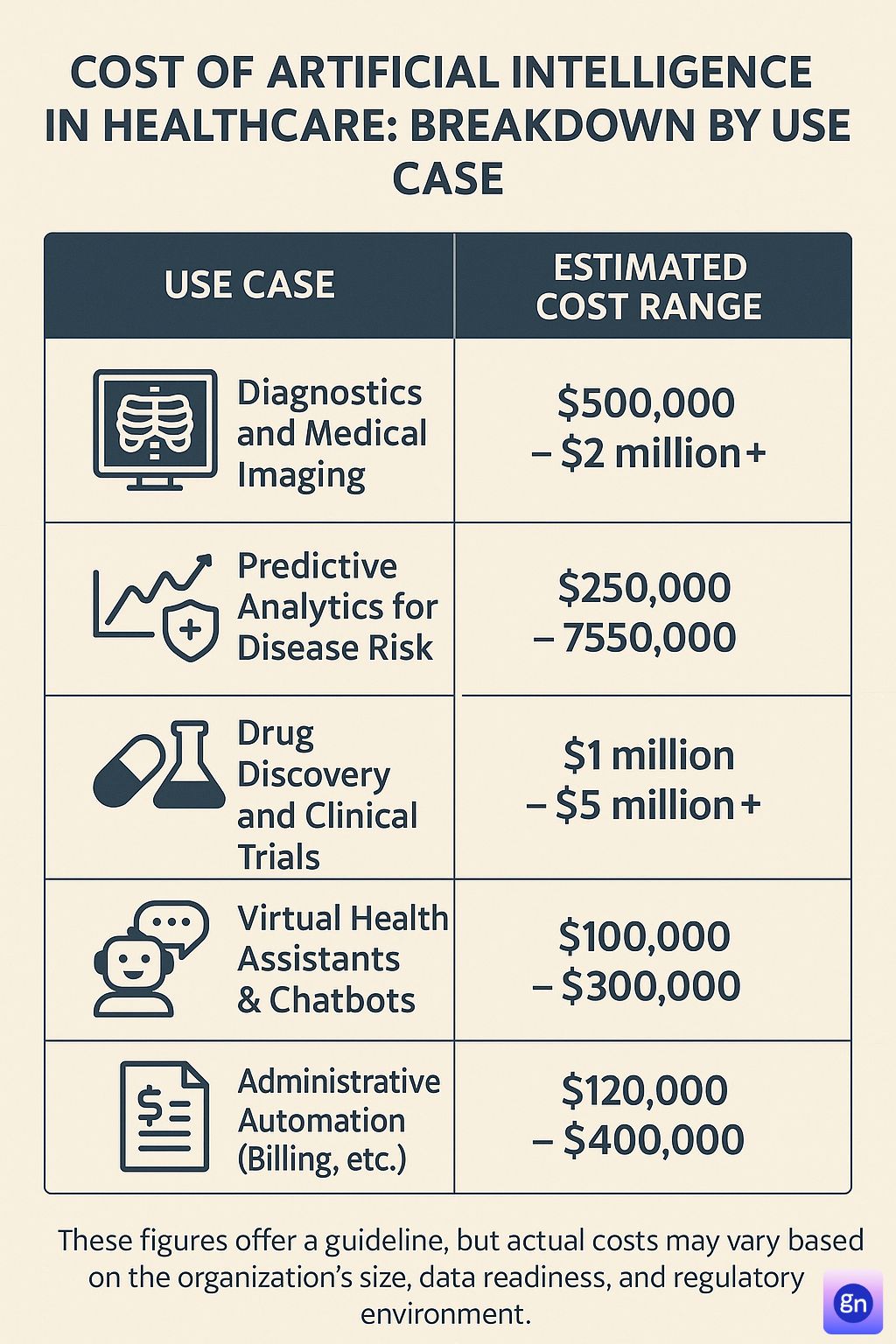
Cost Of Artificial Intelligence In Healthcare: Breakdown by Use Case
The Cost Of Artificial Intelligence In Healthcare isn’t one-size-fits-all. It significantly varies depending on the specific healthcare application being developed or implemented. Understanding these cost variations by use case can help healthcare providers allocate budgets more effectively and choose the most impactful AI solutions for their needs.
1. AI for Diagnostics and Medical Imaging
AI is transforming diagnostics, particularly in fields like radiology, cardiology, and pathology. AI models can detect patterns in X-rays, MRIs, and CT scans faster and sometimes more accurately than the human eye, supporting clinicians in diagnosing conditions such as cancer, fractures, or neurological disorders.
Estimated Cost:
Developing AI models for diagnostic imaging can range from $500,000 to over $2 million, depending on:
- The diversity and volume of training data
- Regulatory requirements for clinical validation
- Integration with Picture Archiving and Communication Systems (PACS)
- Ongoing model retraining to adapt to new imaging data
Incorporating advanced computer vision solutions is often essential in these applications to enable precise image analysis and anomaly detection.
2. Predictive Analytics for Disease Risk and Prevention
Predictive analytics tools help forecast disease progression, hospital readmission risks, and patient deterioration. These tools analyze historical data, genetic information, and lifestyle factors to flag individuals at risk, enabling proactive care.
Estimated Cost:
Custom predictive analytics solutions typically cost between $250,000 to $750,000. This includes:
- Data integration from diverse healthcare sources
- Building predictive models tailored to specific conditions like diabetes or cardiovascular diseases
- Establishing dashboards for healthcare providers to monitor risk indicators
Healthcare institutions leveraging predictive analytics services gain capabilities that not only improve care but also optimize resource utilization.
3. AI for Drug Discovery and Clinical Trials
AI accelerates drug discovery by identifying potential compounds and predicting their interactions, significantly reducing the time and cost involved in bringing new treatments to market. It also enhances the efficiency of clinical trials by selecting optimal participants and predicting outcomes.
Estimated Cost:
Developing AI solutions for drug discovery can range from $1 million to $5 million or more, primarily due to:
- The need for deep learning models trained on extensive biochemical data
- High-performance computing resources
- Collaborative efforts between pharmaceutical researchers and data scientists
Though expensive, the long-term cost savings in R&D and faster drug approvals make this a strategic investment for pharmaceutical companies.
4. Virtual Health Assistants and AI Chatbots
Virtual health assistants support patients with appointment scheduling, medication reminders, symptom checking, and general health inquiries. These solutions improve patient engagement while reducing the administrative burden on healthcare staff.
Estimated Cost:
Implementing AI chatbots or virtual assistants generally costs between $100,000 to $300,000, depending on features, integration with EHR systems, and the complexity of natural language processing capabilities.
To explore solutions in this space, organizations often consult specialists in conversational AI solutions that cater to healthcare-specific communication needs.
5. AI for Healthcare Administrative Automation (Billing, Scheduling, Claims)
AI can automate tedious administrative tasks such as:
- Medical coding and billing
- Claims processing
- Staff scheduling
- Patient record management
Estimated Cost:
Administrative AI solutions typically range from $120,000 to $400,000. The cost largely depends on:
- The number of tasks being automated
- Integration complexity with existing hospital management systems
- Required compliance and data handling standards
AI-driven automation has shown significant potential in reducing operational costs and improving efficiency, a trend supported by Accenture’s research, which estimates AI could save the US healthcare system up to $150 billion annually.
Cost vs. Value: Understanding the ROI of Artificial Intelligence in Healthcare
While the Cost Of Artificial Intelligence In Healthcare can appear high, focusing solely on the upfront investment provides only part of the picture. The return on investment (ROI) from AI adoption often extends beyond immediate cost savings, contributing to better patient outcomes, improved operational efficiency, and long-term financial sustainability.
Reducing Healthcare Costs Through AI Adoption
Healthcare systems globally are under pressure due to rising costs, aging populations, and workforce shortages. According to PwC’s Health Research Institute, healthcare costs in the U.S. are projected to rise by 8% in 2025, making cost-reduction strategies more critical than ever.
AI addresses these challenges by:
- Reducing diagnostic errors that lead to unnecessary tests and treatments
- Enhancing preventive care through predictive analytics, minimizing emergency admissions
- Automating administrative processes to cut labor-intensive tasks
- Optimizing resource allocation within hospitals
A study by Accenture highlighted that combining AI applications across healthcare functions could save the U.S. healthcare economy up to $150 billion annually by 2026. These savings arise from reduced hospital stays, fewer misdiagnoses, and improved management of chronic diseases.
Case Examples Demonstrating Tangible Value
- AI in Radiology: Reduces the time radiologists spend analyzing images, enabling quicker diagnoses and treatment planning, which can shorten hospital stays and improve patient turnover.
- Predictive Analytics in Chronic Disease Management: Hospitals using AI to predict patient deterioration have reported lower readmission rates, which translate into cost savings due to reduced penalties and optimized bed occupancy.
- Administrative Automation: AI solutions in billing and claims processing can drastically reduce manual errors, which in turn lowers claim rejections and improves cash flow for healthcare providers.
These examples show that while the initial Cost Of Artificial Intelligence In Healthcare can be substantial, the value generated over time—both in economic terms and patient care—justifies the investment.
Balancing Costs with Long-Term Gains
The key to maximizing ROI from AI in healthcare lies in:
- Carefully selecting AI use cases aligned with organizational goals
- Starting with a proof of concept to validate effectiveness before scaling
- Ensuring ongoing training and updates to AI models for sustained accuracy
By taking a strategic approach, healthcare providers can ensure that their AI investments deliver both financial and clinical returns, creating a sustainable path toward innovation.
How to Choose the Right AI Model for Your Healthcare Use Case
Choosing the appropriate AI model is a critical decision that directly impacts the Cost Of Artificial Intelligence In Healthcare and the success of its implementation. Selecting the right model ensures not only cost efficiency but also optimal performance aligned with healthcare-specific needs.
1. Define the Problem You Want to Solve
Before diving into AI development, clearly outline the problem or goal. Are you aiming to:
- Improve diagnostic accuracy?
- Predict patient risks?
- Automate administrative workflows?
- Enhance patient engagement with virtual assistants?
Understanding the problem helps in selecting a model that is purpose-built rather than a generic solution, which could lead to unnecessary costs and inefficiencies.
2. Assess Data Availability and Quality
AI models require large volumes of high-quality data to function effectively. If your organization lacks sufficient historical or real-time data, the costs to collect, clean, and label this data can increase significantly.
For data-intensive applications like image recognition or genomics, deep learning models such as convolutional neural networks (CNNs) are often preferred. In contrast, for structured data like patient records or billing information, machine learning models like decision trees or gradient boosting might be more suitable.
3. Evaluate Model Complexity Against Use Case
The complexity of the AI model should match the complexity of the healthcare use case:
- Simple Models: Suitable for tasks like scheduling or basic risk scoring; cost-effective and quicker to deploy.
- Advanced Models: Necessary for complex applications like precision oncology recommendations or multi-modal diagnostic tools, but they come with higher costs in development, training, and maintenance.
Healthcare providers can consult specialized AI audit services to assess the suitability of various AI models against their specific operational goals and data readiness.
4. Consider Explainability and Regulatory Compliance
Healthcare providers must often explain AI-driven decisions to clinicians and patients, especially in critical care scenarios. Models with built-in explainability, such as decision trees or interpretable neural networks, may be favored over black-box systems like some deep learning models.
Additionally, regulatory frameworks may require explainable AI to ensure compliance, especially in regions with stringent data governance laws.
5. Factor in Scalability and Maintenance
Choosing a model that can scale with your organization’s growth is essential. Some models might work well for a pilot project but could become inefficient or costly when scaled across larger datasets or multiple facilities.
When choosing an AI model in healthcare:
- Align complexity with the problem’s demands
- Ensure data availability
- Prioritize explainability for compliance
- Plan for scalability and long-term maintenance
By aligning these considerations, healthcare organizations can control the Cost Of Artificial Intelligence In Healthcare while ensuring the AI solution delivers meaningful and sustainable benefits.
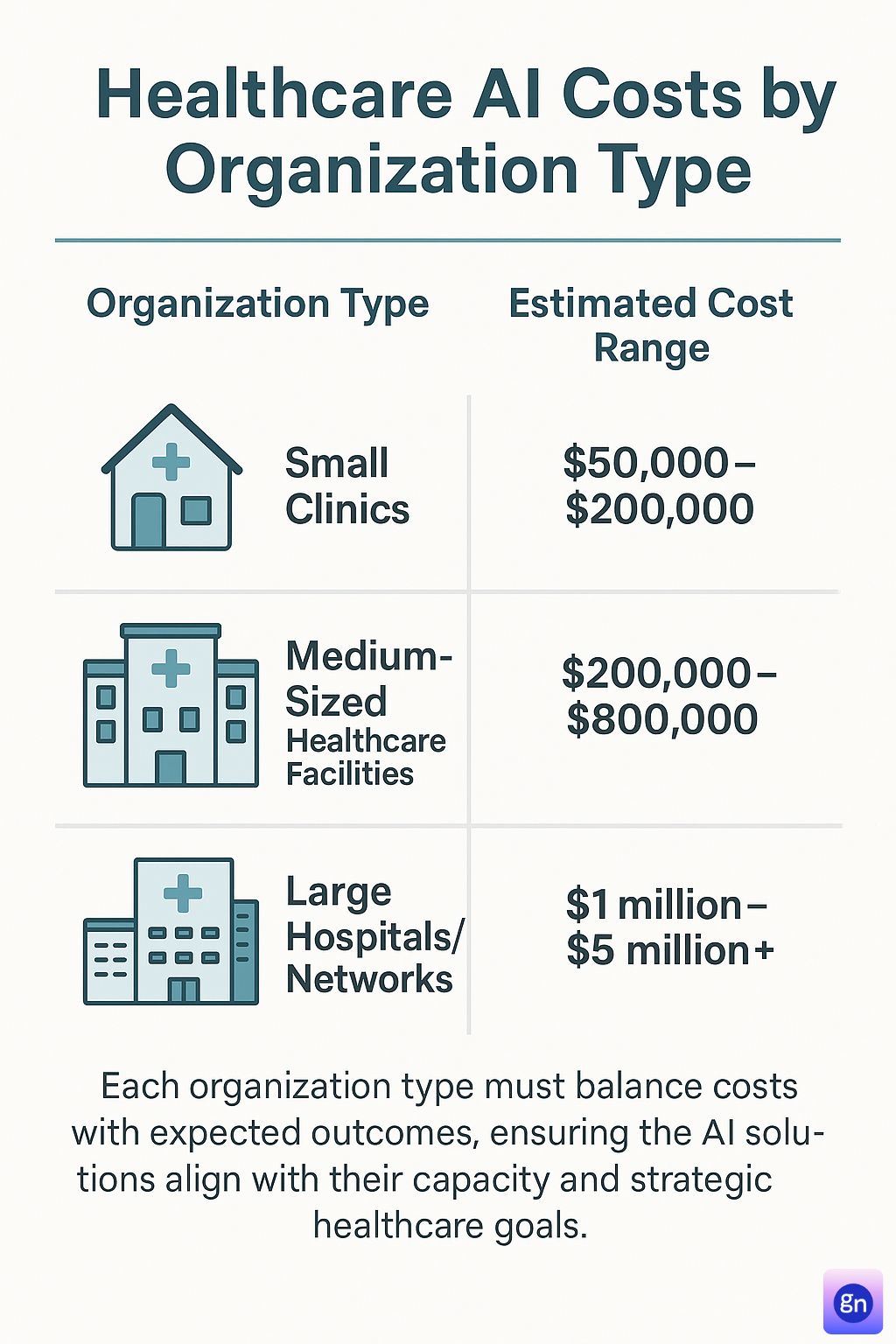
Cost Of Artificial Intelligence In Healthcare: Practical Examples by Organization Type
The Cost Of Artificial Intelligence In Healthcare can vary greatly depending on the type and size of the healthcare organization. Whether you’re a small clinic, a medium-sized healthcare facility, or a large hospital network, your AI investment will differ based on infrastructure, scope, and resource availability.
Understanding these practical cost examples by organization type helps in setting realistic budgets and expectations.
1. Small Clinics
Small clinics often have limited budgets and simpler operational needs. Their primary use cases for AI include:
- Appointment scheduling and patient reminders
- Basic virtual health assistants or chatbots
- Streamlined billing processes
Estimated AI Investment:
Small clinics can expect to spend $50,000 to $200,000 for implementing basic AI solutions. Cloud-based subscription models and off-the-shelf AI tools help reduce upfront costs.
For example, adopting AI-driven chatbots for handling patient inquiries and appointment bookings can reduce administrative workload without significant financial strain. Clinics can further explore AI PoC services to test solutions before scaling.
2. Medium-Sized Healthcare Facilities
These facilities may operate multiple departments and treat a diverse patient population. Their AI needs typically extend to:
- Predictive analytics for patient risk assessment
- Clinical decision support systems
- AI-enhanced diagnostic imaging
Estimated AI Investment:
The investment for medium-sized facilities ranges from $200,000 to $800,000 depending on the sophistication of the solutions. They often need custom integrations with existing Electronic Health Records (EHR) and compliance with local healthcare regulations.
Facilities implementing predictive analytics, such as for anticipating patient readmissions, benefit from long-term cost savings by optimizing resource allocation and improving patient care outcomes.
3. Large Hospitals and Healthcare Networks
Large hospitals and healthcare networks require robust, scalable AI solutions that can handle:
- Advanced diagnostics and imaging analysis
- AI for precision medicine and personalized treatment plans
- Workflow automation across multiple locations
- Comprehensive patient data management and security
Estimated AI Investment:
AI deployment in large healthcare networks typically costs $1 million to $5 million or more. The higher cost is justified by the scale of implementation, the need for highly secure data infrastructure, and continuous model training.
For instance, a hospital network implementing AI for diagnostics, combined with automation in administrative functions, may recoup investments through improved operational efficiency, better patient outcomes, and reduced healthcare delivery costs.
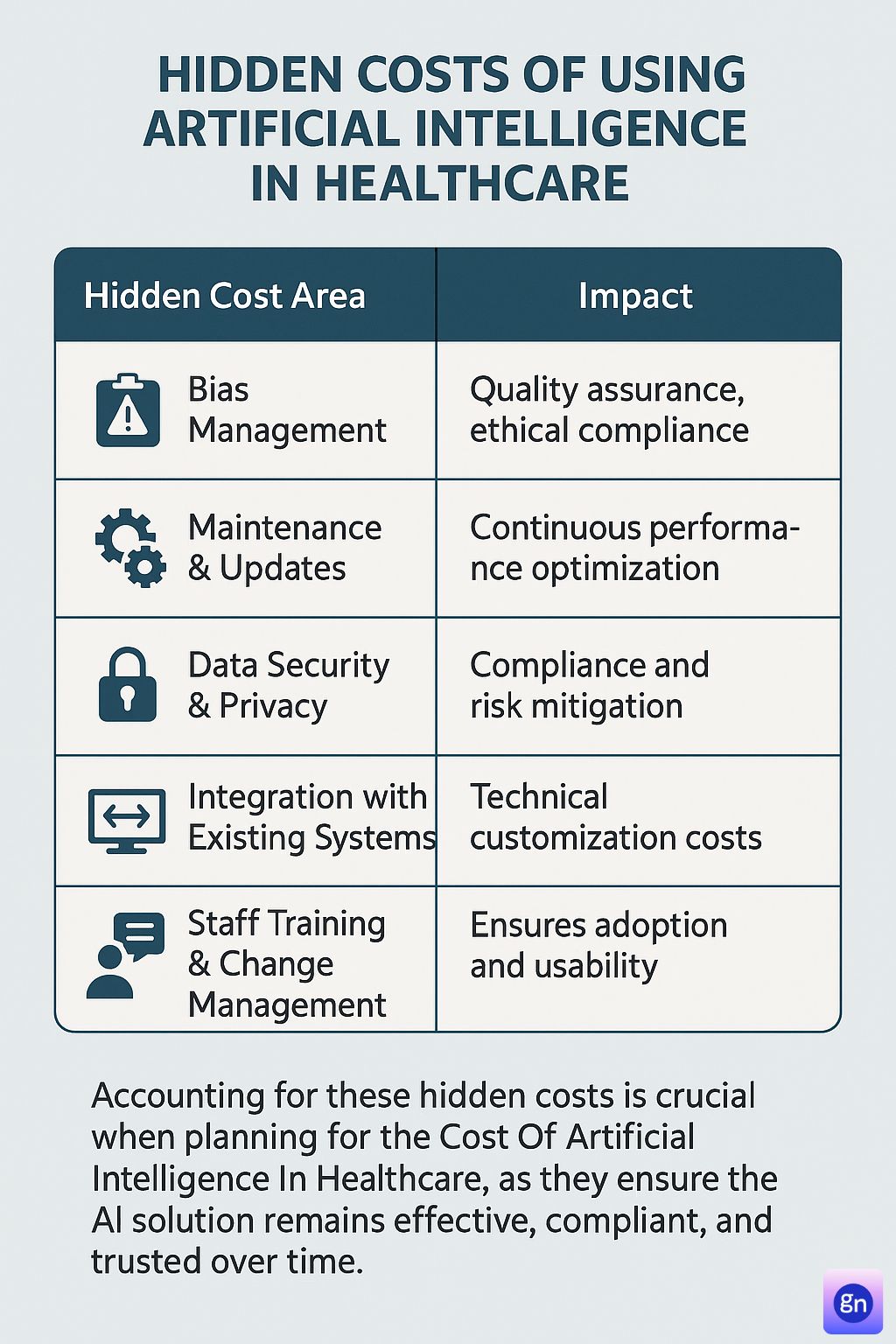
What Are the Hidden Costs of Using Artificial Intelligence in Healthcare?
When evaluating the Cost Of Artificial Intelligence In Healthcare, it’s easy to focus solely on the visible expenses—such as software development, data infrastructure, and implementation. However, hidden costs often emerge during and after deployment, impacting the overall return on investment. Identifying these hidden costs early helps healthcare organizations plan better and avoid unexpected financial strain.
1. Bias Management and Ethical Oversight
AI systems, especially in healthcare, must be trained on diverse, high-quality datasets to avoid biased outcomes. If biases go unchecked, they can lead to inaccurate diagnoses or treatment recommendations, potentially compromising patient safety.
Addressing bias requires:
- Continuous auditing of AI models
- Recruiting domain experts to validate outputs
- Implementing fairness and transparency checks
These activities incur ongoing costs that may not be accounted for during initial planning but are essential for maintaining clinical reliability.
2. Maintenance and Continuous Model Updates
AI models are not static—they need regular updates and retraining to stay effective as new medical data, research, and treatment guidelines emerge. Continuous learning and adaptation are critical in healthcare, where outdated models could lead to poor clinical decisions.
Ongoing maintenance includes:
- Software updates
- Performance monitoring
- Retraining models with new datasets
Budgeting for long-term maintenance is vital to avoid performance degradation over time.
3. Data Security and Privacy Management
Healthcare data is highly sensitive, making data security a critical and often costly component of AI implementation. Ensuring compliance with regulations like HIPAA or GDPR involves investing in:
- Encryption technologies
- Secure data storage solutions
- Regular security audits
Additionally, any data breaches can result in heavy penalties, reputational damage, and patient trust erosion, further adding to indirect costs.
4. Integration Costs with EHR and Legacy Systems
AI solutions must work seamlessly with existing Electronic Health Record (EHR) systems and other healthcare technologies. However, integrating modern AI tools with legacy systems can be complex and resource-intensive, requiring:
- Custom APIs
- Data migration services
- IT consulting support
Integration efforts can lead to unforeseen expenses, particularly if systems are outdated or poorly documented.
5. Staff Training and Change Management
Introducing AI into healthcare workflows often requires training medical staff, administrators, and IT teams to understand and effectively use the new technologies. Costs associated with staff education and change management programs include:
- Training workshops
- Educational resources
- Time invested by staff away from their primary duties
Change resistance is a common barrier, and addressing it through structured training is a hidden but necessary cost to ensure adoption success.
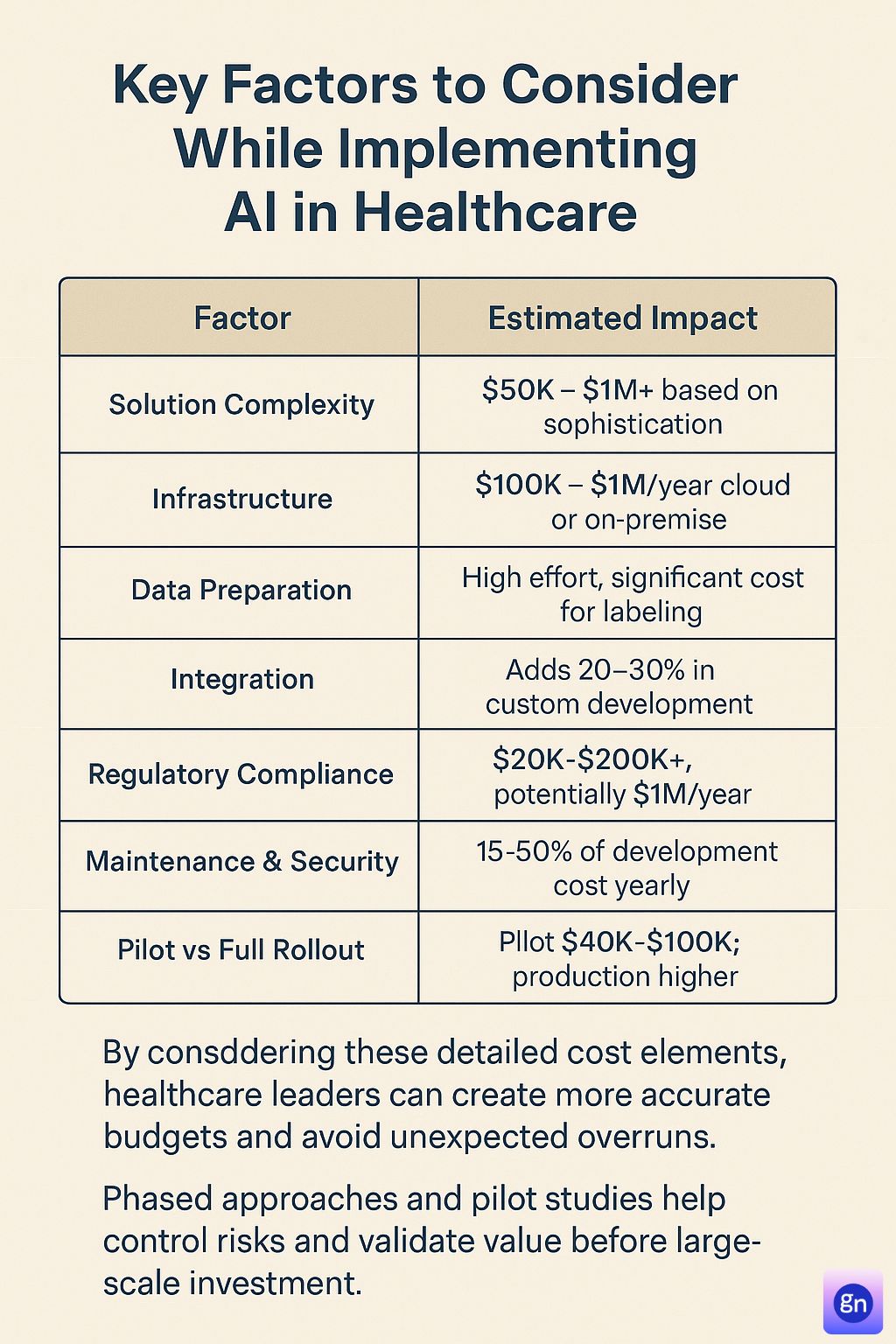
Key Factors to Consider While Implementing AI in Healthcare
Implementing AI in healthcare is more than just a technological upgrade—it requires thoughtful planning, ethical considerations, and strategic alignment with healthcare goals. Beyond the visible Cost Of Artificial Intelligence In Healthcare, healthcare organizations must navigate several key factors to ensure successful and responsible AI adoption.
1. Ethical AI Use
AI in healthcare often deals with life-impacting decisions. Ethical use of AI includes:
- Ensuring transparency in how AI models arrive at conclusions
- Avoiding bias in medical decision-making
- Guaranteeing that AI augments, rather than replaces, clinical expertise
Ethical AI use builds patient trust and aligns with evolving healthcare regulations that demand accountability for AI-driven outcomes.
2. Data Governance and Privacy
Healthcare data is subject to strict privacy laws like HIPAA and GDPR. Effective data governance involves:
- Establishing clear protocols for data usage and sharing
- Maintaining data integrity and accuracy
- Implementing robust cybersecurity measures
Strong data governance not only supports regulatory compliance but also enhances the credibility of AI insights.
3. Skill Requirements and Workforce Readiness
Adopting AI requires healthcare professionals to understand how to interact with AI systems. This includes:
- Training clinicians to interpret AI-generated recommendations
- Upskilling IT teams to manage AI infrastructure
- Educating administrative staff on AI-enabled process changes
Without adequate training, the benefits of AI can be underutilized, leading to poor ROI.
4. Collaboration Between Stakeholders
Successful AI implementation demands collaboration across multiple stakeholders:
- Clinical teams provide domain expertise to guide AI model development.
- Data scientists ensure the accuracy and reliability of AI outputs.
- IT professionals manage system integrations and data security.
Cross-functional collaboration ensures that the AI solution addresses real clinical challenges and integrates smoothly into existing workflows.
5. Scalability and Flexibility
Healthcare needs can evolve rapidly, so AI solutions must be scalable and adaptable to:
- Handle growing data volumes
- Integrate with emerging technologies
- Expand functionalities without major rework
Scalable solutions ensure that the initial investment in AI can yield benefits as the organization grows or diversifies its services.
Checklist for Responsible AI Deployment in Healthcare (with Cost Factors)
| Step | Action | Why It Matters | Associated Cost Factor |
| 1. Define Clear Objectives | Identify specific problems AI will address (e.g., diagnosis, automation, patient monitoring). | Aligns AI investment with measurable outcomes. | No direct cost, but crucial for budget planning. |
| 2. AI Readiness Assessment | Evaluate infrastructure, data quality, and organizational readiness through an AI audit. | Determines feasibility and necessary upgrades. | $10K – $50K for AI audits and assessments. |
| 3. Data Governance & Compliance | Implement policies for data privacy, security, and regulatory compliance (HIPAA, GDPR). | Ensures legal compliance and patient data protection. | $20K – $200K+ annually for compliance and audits. |
| 4. Start with a Proof of Concept (PoC) | Develop a small-scale prototype to validate the AI solution. | Tests ROI and technical viability before scaling. | $40K – $100K for PoC development. |
| 5. Assemble a Cross-Functional Team | Bring together clinicians, data scientists, IT experts, and compliance officers. | Ensures balanced input for clinical relevance and tech efficacy. | Staffing costs vary; typically 15–25% of total project cost. |
| 6. Ethical & Explainable AI | Use models that offer transparency in decisions and avoid bias. | Builds clinician and patient trust; supports regulatory needs. | May require specialized development, adding 10–20% to development costs. |
| 7. Continuous Maintenance & Monitoring | Schedule updates, retraining, and security checks for AI models. | Maintains accuracy and protects against data/model drift. | 15–25% of initial development cost per year. |
| 8. Staff Training & Change Management | Train healthcare teams to integrate AI into their workflows effectively. | Improves adoption rates and minimizes resistance to change. | $10K – $50K depending on organization size. |
| 9. Monitor ROI & Clinical Outcomes | Track key performance indicators like diagnostic accuracy, cost savings, and patient feedback. | Measures success and guides future investment decisions. | Minimal direct costs; requires dedicated team time and analytics tools. |
| 10. Scale Gradually | Expand AI solutions incrementally across departments or facilities. | Controls budget and allows performance evaluation before full-scale rollout. | Cost depends on scale; progressive scaling minimizes risks. |
Key Takeaway
By considering these steps with associated cost factors, healthcare providers can better estimate the Cost Of Artificial Intelligence In Healthcare while ensuring ethical use, compliance, and measurable value.
Cost Variations Based on Different AI Applications in Healthcare
The Cost Of Artificial Intelligence In Healthcare varies significantly depending on the type of AI application being developed or implemented. Each healthcare domain has different complexities, data requirements, and regulatory implications, all of which contribute to the cost differences.
Here’s a breakdown of typical AI applications in healthcare along with their estimated cost ranges:
| AI Application | Purpose | Estimated Cost Range | Cost Drivers |
| AI for Diagnostics & Medical Imaging | Analyze X-rays, MRIs, CT scans for detecting diseases like cancer, fractures, etc. | $500,000 – $2 million+ | Large labeled datasets, regulatory approval, integration with imaging devices |
| Predictive Analytics for Disease Risk | Predict risk of chronic diseases, patient deterioration, or hospital readmissions. | $250,000 – $750,000 | Data integration from multiple sources, model complexity, ongoing retraining |
| Drug Discovery & Clinical Trials Optimization | Identify potential drug compounds and optimize clinical trials through AI. | $1 million – $5 million+ | Advanced deep learning models, extensive R&D, high-performance computing |
| Virtual Health Assistants & AI Chatbots | Support patients with symptom checking, medication reminders, and appointment scheduling. | $100,000 – $300,000 | Natural language processing, conversational AI development, integration with health records |
| Administrative Automation (Billing, Scheduling, Claims) | Automate repetitive tasks like billing, insurance claims processing, and scheduling. | $120,000 – $400,000 | Customization to existing hospital management systems, data security needs |
Key Cost Influencers Across Applications
- Data Requirements: More complex data (e.g., medical images vs text data) drives up costs.
- Model Complexity: Simple machine learning models are cheaper than deep learning or multimodal models.
- Compliance Needs: Solutions involving direct patient care require more regulatory scrutiny, increasing costs.
- Integration Needs: AI that must interact with legacy hospital systems requires more development time and expense.
Cost Planning Insight
Understanding the intended application helps healthcare providers align their budget accurately. For instance:
- A small clinic looking to automate appointment scheduling may only need a $100K–$200K investment.
- A hospital aiming to deploy AI-driven diagnostics might need to plan for a multi-million-dollar budget, factoring in ongoing maintenance and compliance.
Strategies to Optimize Your Investment in Artificial Intelligence in Healthcare
Given the significant Cost Of Artificial Intelligence In Healthcare, adopting smart investment strategies is essential to maximize value while minimizing unnecessary expenses. Healthcare providers can apply these practical approaches to ensure their AI initiatives are both cost-efficient and outcome-driven.
1. Start with a Proof of Concept (PoC)
Launching a PoC allows organizations to test an AI solution’s feasibility, clinical relevance, and technical performance before committing to a full-scale rollout. A PoC typically costs between $40,000 to $100,000, depending on complexity.
Benefits:
- Identifies technical and clinical challenges early
- Minimizes risk of large-scale financial loss
- Provides measurable insights into potential ROI
Partnering with services like AI PoC solutions can help healthcare organizations structure and evaluate pilot projects effectively.
2. Leverage Cloud-Based Solutions
Choosing cloud infrastructure over on-premise hardware reduces upfront capital expenditure and allows for scalable costs as usage grows. Cloud platforms also offer built-in compliance features for data security and privacy, reducing the cost of custom security implementations.
Cost Impact:
Cloud solutions typically shift costs from capital expenditure (CapEx) to operating expenses (OpEx), offering greater flexibility in budgeting.
3. Select Pre-Trained Models Where Applicable
Not every healthcare application requires a fully custom AI model. For tasks like image recognition or text summarization, pre-trained models can significantly lower development costs and time-to-deployment.
Cost Savings:
Using existing frameworks or APIs can reduce AI development costs by 30–50% compared to building solutions from scratch.
4. Collaborate with AI Solution Providers
Partnering with experienced AI vendors allows healthcare organizations to leverage established expertise, tools, and methodologies. Vendors often provide bundled services like audits, development, and compliance consulting, streamlining the process.
Providers such as GlobalNodes offer tailored AI solutions that align with both clinical goals and budget constraints.
5. Implement Incremental Scaling
Instead of a full-system deployment, roll out AI in phases:
- Start with a single department or use case
- Monitor performance and outcomes
- Gradually expand across other areas
This approach helps control costs, manage change effectively, and adapt strategies based on real-world feedback.
6. Optimize Data Strategy
Investing in a solid data strategy reduces long-term costs by:
- Ensuring data is clean, structured, and ready for AI model consumption
- Streamlining data integration with EHR and other systems
- Reducing redundant data processing efforts
Good data governance can prevent costly errors and rework in AI model training and deployment.
7. Plan for Long-Term Maintenance and Updates
Allocating a portion of the budget for ongoing maintenance, model retraining, and system updates is critical. Without this, AI models risk becoming outdated, leading to poor performance and potential compliance issues.
Expected Maintenance Cost:
Typically, set aside 15–25% of the initial project cost annually for updates and support.
Summary of Cost-Optimization Strategies
| Strategy | Estimated Savings/Impact |
| Proof of Concept (PoC) | Saves up to 60% on initial large investments |
| Cloud-Based Deployment | Reduces CapEx, enables flexible scaling |
| Use of Pre-Trained Models | Lowers development cost by 30–50% |
| Vendor Collaboration | Streamlines development & compliance |
| Incremental Scaling | Controls budget while improving adoption |
| Data Strategy Optimization | Prevents costly rework in data handling |
| Maintenance Planning | Sustains performance, reduces long-term risks |
Implementing these strategies ensures healthcare organizations can manage the Cost Of Artificial Intelligence In Healthcare effectively while maximizing clinical and financial outcomes.
Funding and Pricing Models for Artificial Intelligence in Healthcare
The Cost Of Artificial Intelligence In Healthcare varies not only by the solution but also by the financial strategies and funding models that healthcare organizations adopt. For healthcare providers in the USA, India, and other markets, understanding the available pricing and funding options is critical to make AI adoption financially sustainable.
1. Upfront Investment Model
This model involves a one-time capital expenditure to develop, customize, and deploy an AI solution. It’s often used by large hospitals, healthcare networks, and research institutions that have the resources for significant upfront investment.
Typical Cost Range:
- USA: $500,000 to $5 million+
- India: ₹1 crore to ₹20 crore+
Best For:
- Large hospital networks
- Pharmaceutical companies
- Research-intensive healthcare organizations
Pros:
- Full ownership of the AI system
- Greater control over data and customization
Cons:
- High initial financial risk
- Longer time to ROI
2. Subscription / SaaS (Software-as-a-Service) Model
In this model, healthcare providers pay a recurring monthly or annual fee to use AI tools hosted on the cloud. This pricing model is particularly attractive for:
- Small to medium-sized clinics
- Diagnostic centers
- Outpatient services
Typical Cost Range:
- USA: $5,000 to $30,000 per month
- India: ₹4 lakh to ₹20 lakh per month
Pros:
- Lower upfront costs
- Easier to scale with needs
- Regular updates and support included
Cons:
- Ongoing operational expenses
- Less customization than bespoke solutions
3. Performance-Based Pricing
Some AI vendors offer pricing models tied to the outcomes or efficiencies delivered by the AI solution. For example, payment may be based on:
- The number of diagnostic errors reduced
- Time saved in hospital operations
- Increase in patient throughput
This model is increasingly popular in value-based healthcare frameworks, particularly in the USA, where providers are incentivized for better outcomes.
Best For:
- Providers focused on ROI-driven investments
- Hospitals participating in value-based care programs
4. Government Grants and Public Funding
Both India and the USA have public funding opportunities to support healthcare innovation:
- USA: NIH, NSF, and Department of Health and Human Services offer grants for AI research in healthcare.
- India: Programs under NITI Aayog and Digital India promote AI in healthcare through funding, policy support, and collaborations with private tech companies.
Securing such grants can significantly offset the Cost Of Artificial Intelligence In Healthcare, particularly for research-driven projects or public health applications.
5. Public-Private Partnerships (PPPs)
In emerging economies like India, PPPs enable collaboration between government bodies and private technology firms to co-develop AI solutions for healthcare at a shared cost. This model is effective for deploying AI in public health systems where budgets are constrained but scale is large.
6. Collaborative Partnerships with AI Vendors
Instead of outright purchases, many organizations partner with AI vendors through:
- Revenue-sharing models
- Joint ventures
- Customized pricing based on service scale
Vendors like GlobalNodes offer flexible partnerships that align with organizational goals, reducing the financial burden while ensuring strategic alignment.
Summary of Funding & Pricing Models
| Model | Typical Cost | Ideal For |
| Upfront Investment | $500K–$5M+ / ₹1–20 Cr | Large hospitals, pharma, research |
| Subscription / SaaS | $5K–$30K/month / ₹4–20L | Clinics, diagnostics, SMEs |
| Performance-Based Pricing | Varies based on outcomes | Value-based care providers |
| Government Grants | Partial/full funding | Public hospitals, research orgs |
| Public-Private Partnerships | Shared costs | Public health systems, India focus |
| Vendor Partnerships | Customized pricing | Diverse healthcare providers |
Cost of Implementing AI in Healthcare: Is It Worth Investing in Artificial Intelligence?
When considering the Cost Of Artificial Intelligence In Healthcare, healthcare providers often ask: Is the investment worth it? The short answer is: yes, if approached strategically. While the initial costs can be significant, the long-term benefits—both financial and clinical—can far outweigh the expenditure.
Long-Term Financial Benefits
AI solutions offer measurable financial advantages by:
- Reducing operational inefficiencies: AI automates tasks such as medical billing, appointment scheduling, and claims processing, reducing administrative overhead.
- Minimizing diagnostic errors: Early detection of diseases like cancer through AI-powered imaging reduces treatment costs and litigation risks.
- Optimizing resource utilization: Predictive analytics help hospitals manage bed capacity, staff allocation, and medical supplies efficiently.
Case in Point:
Accenture’s research suggests that AI applications could save the U.S. healthcare system $150 billion annually by 2026. Similarly, in India, AI is streamlining public healthcare and reducing disparities in rural health access, as supported by NITI Aayog’s AI policy initiatives.
Clinical Value and Better Patient Outcomes
AI enhances patient care through:
- Personalized treatment plans: AI can analyze genetic data and medical history to tailor therapies.
- Improved patient monitoring: Wearables combined with AI can alert clinicians to early signs of deterioration.
- Faster diagnosis and treatment: AI accelerates analysis of medical images and lab results.
These improvements directly contribute to better health outcomes, shorter hospital stays, and increased patient satisfaction.
Strategic Value in Competitive Healthcare Markets
For private hospitals and healthcare startups, investing in AI also offers:
- Market differentiation: Hospitals adopting AI stand out as technology-forward institutions.
- Attracting partnerships: AI capabilities can attract research collaborations and funding from both public and private sectors.
In both USA and India, healthcare providers incorporating AI are better positioned to thrive in increasingly competitive and value-driven markets.
Balancing Costs with Returns
While developing custom AI solutions may cost between $100,000 to several million dollars, organizations can:
- Start small with targeted AI applications (e.g., chatbots or scheduling assistants)
- Scale gradually as ROI is proven
- Explore subscription models or partnerships to lower initial costs
By managing costs with scalable strategies and focusing on high-impact areas, the investment in AI becomes not just justified, but necessary for future-ready healthcare.
Conclusion
Though the Cost Of Artificial Intelligence In Healthcare may seem substantial initially, the long-term benefits—increased efficiency, reduced costs, improved care quality, and competitive advantage—make it a worthwhile investment for healthcare providers globally. When planned carefully, AI can drive both clinical excellence and financial sustainability.
Cost Of Artificial Intelligence In Healthcare: FAQs
1. How much does it cost to implement AI in a hospital?
The Cost Of Artificial Intelligence In Healthcare for hospitals can range from $500,000 to over $5 million, depending on the complexity of the solution, data requirements, and scale of implementation. Smaller AI applications like virtual assistants or appointment scheduling tools may cost around $100,000 to $300,000.
2. What are the main cost factors for AI in healthcare?
The primary factors influencing the cost include:
- Complexity of the AI solution
- Data acquisition and preparation
- Infrastructure (cloud vs on-premise)
- Integration with existing healthcare systems
- Regulatory compliance (HIPAA, GDPR)
- Ongoing maintenance and retraining needs
- Staff training and change management
3. Can AI reduce healthcare costs in the long run?
Yes. AI can significantly reduce healthcare costs by:
- Automating administrative tasks
- Reducing diagnostic errors
- Enhancing preventive care with predictive analytics
- Optimizing hospital resource management
For example, research by Accenture suggests that AI could save the U.S. healthcare system up to $150 billion annually by 2026.
4. Are there affordable AI options for small healthcare providers?
Absolutely. Small clinics and diagnostic centers can implement affordable AI solutions through:
- Subscription-based SaaS models
- Pre-trained AI tools
- Limited-scope solutions like chatbots or patient engagement platforms
These options typically cost between $50,000 to $200,000, making AI accessible even to smaller providers.
5. What funding options are available for AI in healthcare?
Healthcare organizations can explore:
- Government grants and subsidies: Available in countries like the USA (NIH, NSF) and India (NITI Aayog initiatives).
- Public-private partnerships: Especially effective in developing economies.
- Vendor partnerships and revenue-sharing models: Offered by many AI service providers.
- Performance-based pricing: Where payment is linked to achieved outcomes.


